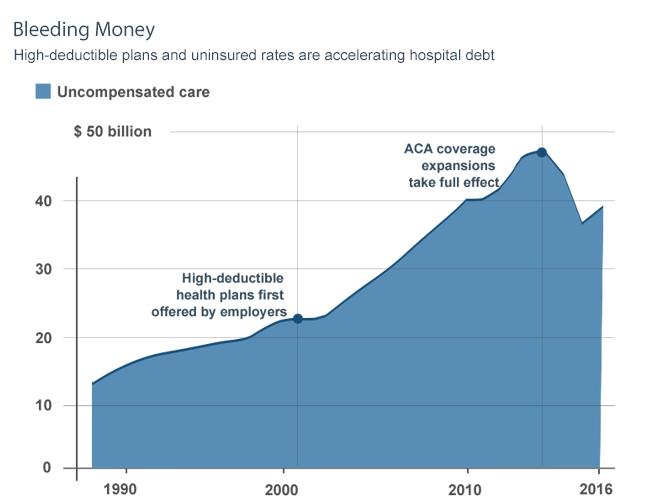
There was a time when doctors, healthcare providers, and medical labs had to worry about receiving payments from the patients without insurance coverage. Now, times have changed, and healthcare providers are more concerned about receiving payments from those who have insurance. Over the last decade, employers and insurers have been shifting the cost of care onto their customers and workers.
This is being done by reducing the annual premiums but increasing the patients' out-of-pocket costs. According to the government data published last year, almost half of the privately insured Americans under the age of 65 had an average annual deductible in the range of $1300 - $6550.
Current Scenario - How Medical Bill Collection Process Has Changed Over the Years
Instead of getting paid from the insurance company on a fixed schedule, the doctors and healthcare providers are stuck in an awkward situation between the patients and the insurance companies. At one moment they are treating a deadly disease and at the next moment they are engaging in long conversations with the patients and asking them to pay for the treatment bill.
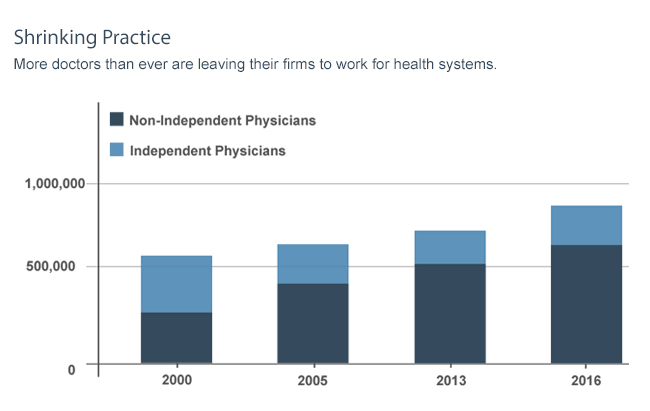
Doctors have claimed that it is more difficult to get the payments from the patients as compared to the insurance companies. It makes it even more difficult to get the payments from the patients if the plans change to higher annual deductibles. The reimbursement pressures have raised several questions on independent physicians whether to stay in business or not.
What are the Solutions Being Adopted to Tackle this Problem?
Back in 2016, several schemes were introduced to help patients with medical bill payments. Once such scheme was allowing the patients with expensive plans to pay a portion of the amount upfront on a monthly basis over the course of several years. This scheme didn't do as well as expected as the number of people avoiding the payments calls increased after the treatment was completed.
Another option that was introduced was wherein the patients were given the billing codes before the procedure was conducted. They could approach the insurance companies and get the estimates of the treatment and plan the procedure accordingly. The collection rates were comparatively slower for this program too, especially during the beginning of the year when the deductibles were reset.
Is it Fair for Doctors to Double Up as Debt Collectors?
These challenges are forcing non-independent doctors and physicians to give up their business and joining other medical groups or larger healthcare organizations as they offer better security and additional benefits. Doctors are caught between patients who are not able to pay their medical bills and insurance companies who are ready to cover for the patients more than what is required of them. This is completely unfair.
So what is the next step that doctors and independent physicians need to take? The next best step would be to outsource these mundane admin tasks to an experienced service provider. By outsourcing, doctors and healthcare organizations will not only streamline the process of medical billing and improve their cash flow but also have an ample amount of time to focus on patient care.
Choose Flatworld Solutions for Cost-effective and Efficient Medical Billing & Coding Services
Flatworld Solutions has been a pioneer in providing quality medical billing and coding services and a plethora of other healthcare services to doctors and independent physicians across the globe. Our team comprises some of the most talented and skilled medical billing and coding experts who will relieve you of all your back-office tasks and help you focus better on patient care.
We have the required skills and expertise to provide several back-office services such as insurance eligibility verification, accounts receivable follow-up, medical billing charge entry, CPT and ICD-10 coding, patient demographic entry, denial analysis, etc. If you are looking for a reliable, cost-effective, and efficient medical billing and coding service provider, then you have come to the right place. Get in touch with us today!
Our Customers





Key Differentiators
AHIMA Healthcare Convention 2016

USA
Flatworld Solutions
116 Village Blvd, Suite 200, Princeton, NJ 08540
PHILIPPINES
Aeon Towers, J.P. Laurel Avenue, Bajada, Davao 8000
KSS Building, Buhangin Road Cor Olive Street, Davao City 8000
INDIA
Survey No.11, 3rd Floor, Indraprastha, Gubbi Cross, 81,
Hennur Bagalur Main Rd, Kuvempu Layout, Kothanur, Bengaluru, Karnataka 560077















